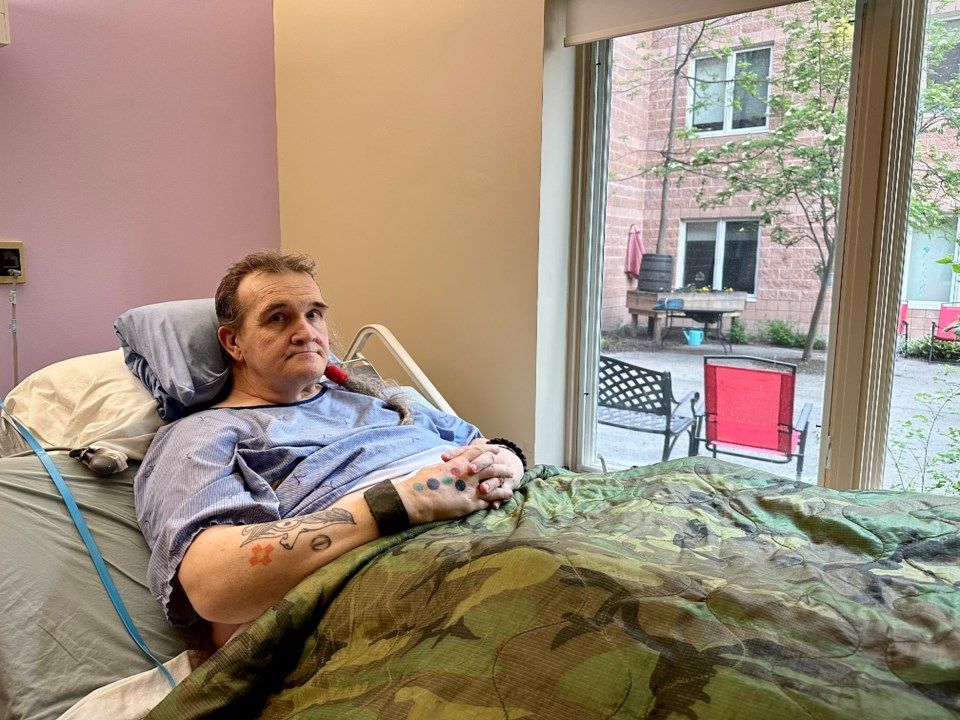
A long-term care resident at the Leacock Care Centre recently had to sit in his own excrement overnight as his pleas for help could not be answered due to staffing issues.
Resident Dav Langstroth, 69, suffers from incontinence and no longer has the ability to use his lower body. He sat in his waste from 10:30 p.m. on May 22 until 6 a.m. on May 23, when he received the care he needed.
He said a shortage of staff led to the situation, adding it typically requires two people to change him.
“I had a bowel movement, rang the call bell; staff came in,” Langstroth told OrilliaMatters. “The night (personal support worker) said, ‘I can’t change you because I don’t have another person to help me.’”
Staff apologized to him the following morning, he said, but he questioned why there were not enough workers present to address his needs.
“Six o’clock (in the) morning, the staff came in and said, ‘We’re really sorry about having you sit in your (waste) all night, but we didn’t have any staff,’” he said. “I’m going, ‘Well, why didn’t you?’ And I was told that there was another nurse here — they could have provided help.”
Langstroth has stayed at the for-profit home since December 2022. He said he has previously had to wait up to a couple of hours to be changed, but May 22 was the “straw that broke the camel’s back.”
“I’m finding this to be a situation where it’s no longer tenable for me,” he said. “There have been other nights, many nights, when people couldn’t change me because, again, (there’s) one person on.”
He has suffered both mental and physical anguish as a result of the incident, as his waste became like a “mild acid” on his body, causing pain and discomfort, which led to an “extremely painful” process when he finally received care.
He said he has few issues with the staff at Leacock Care Centre, noting they do their best to carry out their work under trying circumstances.
“They’re usually pretty much on the ball,” he said. “It can be two, three hours sometimes because staff are busy (with) other people … Last night it was eight hours, basically, and I’m finding that not tenable. It’s damaging to me physically and mentally.”
However, he questions what’s being done at the administrative level.
“There are people that are burning out left, right and centre,” he said of front-line staff.
Some staff occasionally work double shifts, he said, to try to meet demand.
“Somebody from senior staff says, ‘Oh, so-and-so’s not coming in tonight. Can you do a double?’ That’s quite common,” he said.
“There’s not enough qualified people, and the administration is making it more and more difficult, and that’s because of cost-cutting. It’s not unusual on weekends to eat off of Styrofoam plates because they don’t have the staff to wash the dishes.”
He said he has chosen to speak out on the situation on behalf of others, as well, who might have difficulty advocating for themselves.
“It’s dehumanizing, but (this is) not so much for me. It’s for all the other people that can’t make that communication,” he said. “If that level of care is not being done for me, what is not being done for other people who don’t have a voice?”
Due to the outlook of his physical limitations, Langstroth said he has begun the process for medical assistance in dying (MAID), which he hopes can take place this fall.
“I have applied for a MAID certificate to end this endless nightmare of shitting, pissing and doing nothing all day,” he said.
He said he has filed complaints with regard to the May 22 incident.
Trevor Sykes, community relations co-ordinator for Jarlette Health Services, said the company takes every complaint seriously.
“Our primary concern, each and every day, is the health, safety and well-being of our residents,” he told OrilliaMatters in a statement. “We take every complaint and concern brought to our attention very seriously. We are not able to comment on the personal care of individual residents.”
However, he said an investigation has been undertaken in response to complaints made by a resident.
“Our team members are in direct and regular contact with the resident to ensure they are receiving proper care, and to confirm that their concerns are being addressed in a timely manner,” Sykes said. “We have made all mandatory reports to our regulatory authorities and we are actively following up with the resident throughout the course of the investigation.”
Jarlette Health Services, which owns and operates Leacock Care Centre, did not respond to questions about staffing levels or the frequency of such incidents.
Leacock Care Centre officials declined to comment for this article.
Upon reading about Langstroth's experience, Long-Term Care Minister Paul Calandra said in a statement that the conditions described at Leacock Care Centre "are unacceptable."
"The Ministry of Long-Term Care will be conducting an inspection of the home to ensure any and all instances of non-compliance are corrected as quickly as possible," he said. "Any home that fails to meet the care standards set out in the Fixing Long-Term Care Act is subject to corrective actions, which could include written notifications, administrative monetary penalties, and compliance orders. Repeated instances of non-compliance will result in escalating penalties, which could include mandatory management and cease of admissions orders."